Diabetic Nephropathy: Can Stem Cell and Exosome Therapy Help?
Clinical Insights by Prof. Dr. Serdar Kabataş, MD, PhD (C)
Clinical Perspective on Diabetic Nephropathy
I’m Prof. Dr. Serdar Kabataş, and for more than two decades I have worked with diseases that do not always introduce themselves dramatically.
Diabetic nephropathy is one of them.
It rarely begins with a scene.
No panic.
No memorable day.
No single moment patients point to and say: that was the start.
It usually builds behind the routine.
Diabetic nephropathy stem cell therapy becomes relevant only when patients begin asking how much kidney function can still be protected.
A patient lives for years with diabetes that is “more or less fine.” Another has blood sugar that improves, then slips, then improves again. Someone else feels generally well and pays attention only when the urine changes or the kidney numbers stop looking harmless.
That is how diabetic kidney disease usually appears.
Quietly.
Gradually.
With very little theater.
And that is part of the problem.
I remember a patient asking me, “If my kidneys are already involved, am I already too late?” I have heard versions of that question many times. Most patients are aware that diabetes can damage the kidneys. However, they usually do not know what can be done about it, whether anything can be done at all, or whether it is already too late to do anything about it.
That is where the real discussion starts.
Because diabetic nephropathy is not just a story of numbers drifting in the wrong direction. It is a story of tissue that has been sitting under metabolic pressure for years. Vascular strain. Inflammation. Repeated biochemical stress. And once that pattern is established, the question changes.
It is no longer only how the damage happened.
It becomes whether the environment inside the kidney can still be pushed in a less destructive direction before too much has been lost.
That is why regenerative medicine enters the conversation at all.
Not as a cure.
Not as an excuse to relax diabetic care.
But as a serious biological question.
Table of Contents
What Diabetic Nephropathy Actually Is
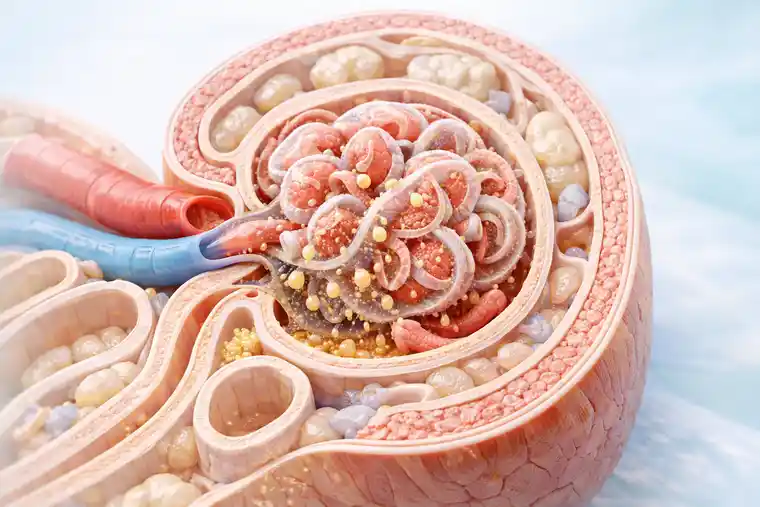
Diabetic nephropathy means kidney damage caused by diabetes over time.
That sounds straightforward. In real patients, it is not.
The kidney is packed with delicate filtering structures and very small vessels. Diabetes does not destroy them in one dramatic event. It works more slowly than that. The tissue is exposed again and again to unstable glucose, vascular dysfunction, inflammatory activity, and abnormal signaling. At first, the changes may be subtle. Later, they stop being subtle.
Patients often hear first about protein in the urine, long before they understand what that really means.
It matters because the kidney is starting to leak.
And when the kidney starts to leak, it is telling us the filtering barrier is under stress.
That does not automatically mean dialysis is close. However, something is happening, that should not be ignored.
Why Diabetic Nephropathy Is Different From Other CKD Causes
Not every case of chronic kidney disease follows the same course.
A patient with diabetic nephropathy may experience very different problems from someone who also has kidney disease but for a different reason. Kidney disease can also be caused by high blood pressure, or possibly by an immune reaction, or even by a reaction to medication. There can be overlap, of course. Often there is. But diabetes brings its own pattern.
The damage is structural, yes.
But not only structural.
- It is metabolic.
- It is vascular.
- It is inflammatory.
That mix is what makes diabetic nephropathy so difficult.
The kidney is not just being scarred. It is being stressed by the same broader disease that caused the injury in the first place. That is why some patients continue to worsen even while daily life still feels more or less normal. The biology stays active much longer than symptoms announce.
And that is one reason diabetic nephropathy keeps coming up in regenerative medicine discussions.
Why Patients Often Notice It Late
One of the hardest things about diabetic kidney disease is that people often do not feel it while it is getting started.
They may feel tired, but diabetes itself can do that for many reasons. They may have higher blood pressure, some swelling, a change in labs, but nothing that creates one clear alarm bell. In many patients, diabetic nephropathy shows itself first in testing, not in sensation.
That delay changes how the diagnosis lands.
Patients often think in extremes.
Either everything is fine, or kidney failure has already begun.
Usually the truth is somewhere in the middle.
And that middle is exactly where decisions matter most.
Can Diabetic Nephropathy Be Reversed?
This is usually the first real question, even when it is not asked in those exact words.
Usually not completely.
If fibrosis and structural damage are already established, full reversal is not a realistic goal. The kidney does not go back to an untouched state just because glucose improves or because a new treatment enters the picture.
But that still leaves a lot of ground between “normal again” and “nothing can be done.”
Those are not the same thing.
In diabetic nephropathy, the more realistic aim is usually to slow the process, reduce the ongoing injury, protect what function is still there, and delay more advanced loss as long as possible.
That may sound modest from the outside.
To a patient trying to stay away from dialysis, it usually does not sound modest at all.
Why Stem Cell Therapy Is Being Discussed in Diabetic Nephropathy
Regenerative therapy is being discussed in relation to many conditions. This is particularly important in the case of diabetic nephropathy, which is one of the most important forms of chronic kidney disease. Here are several things at once that damage the kidneys.
- The kidney is sitting under metabolic stress.
- The small vessels are affected.
- Inflammatory signaling keeps going.
- Fibrotic pathways do not simply switch themselves off.
That creates a situation in which standard care remains essential, but also one in which it becomes reasonable to ask whether the tissue environment itself can still be influenced.
That is where stem cells and exosomes enter the conversation.
Not because they can manufacture a new kidney.
Not because they erase diabetic damage.
But because they may affect the inflammatory and signaling conditions in which the damage continues.
That is really the point.
The idea is preservation.
Not replacement.
Can Stem Cell Therapy Help in Diabetic Nephropathy?
Possibly, in selected patients.
That is the honest answer.
The interest in stem cell therapy for diabetic nephropathy comes mostly from its potential immunomodulatory and paracrine effects. Put more plainly, the hope is that treatment may reduce some of the harmful signaling and inflammatory pressure that continue to injure the kidney.
That difference matters for patients.
Many hear “stem cell therapy” and immediately picture rebuilding. That is not really the right picture here. The more serious question is whether stem cells may help create a less hostile environment around the tissue that is still alive and still working.
That is a narrower claim.
It also happens to be a much more believable one.
Where Exosomes Fit In
Exosomes are often mentioned together with stem cells, and in diabetic nephropathy there is a reason for that.
This is a disease driven by disturbed cellular signaling over time. The kidney is not failing because one switch suddenly flipped in one afternoon. It is being pushed, repeatedly, by stress, inflammatory activity, vascular dysfunction, and communication that has gone wrong.
That is why exosomes matter in the discussion.
Not because they sound futuristic.
Because the disease itself is tied to signaling.
So yes, exosome-based approaches belong in the same broader regenerative conversation. But the language still has to stay under control. Patients should not hear “exosomes” and imagine precision repair that has already been proven. They should hear something more restrained: this is a biologic strategy being explored for its signaling effects, not a guaranteed answer.
Which Patients May Be Better Candidates for a Serious Discussion?
Not every patient with diabetic nephropathy is standing in the same place, even when the diagnosis sounds identical.
One patient has early kidney involvement, albumin in the urine, and enough reserve left that protection still means something. Another has had diabetes for many years, has more established scarring, shows declining kidney function over repeated follow-up, and already carries several later complications in the background.
Those are different conversations.
The first patient may justify a more ambitious preservation discussion.
The second may still deserve a thoughtful conversation, but the tone usually changes. Less about changing the slope dramatically. More about preserving function, limiting damage, and not pretending the window is wider than it really is.
That is why selection matters so much.
The label alone is not enough. What matters is whether the disease is still active, how much fibrosis is already there, and how much usable reserve remains.
Standard Diabetic and Kidney Care Still Comes First
This has to be said plainly.
No regenerative therapy compensates for uncontrolled diabetes.
If glucose remains poorly managed, blood pressure is neglected, medication is inconsistent, and kidney follow-up is loose, then the main injury is still happening. In that setting, even the most biologically interesting treatment is being asked to work against damage that has not actually been brought under control.
That is not a serious strategy.
In diabetic nephropathy, standard care still does the real work:
- blood sugar control
- blood pressure control
- reduction of albuminuria
- protection from additional kidney stress
- regular nephrology follow-up
Regenerative therapy, where it is discussed, has to rest on top of that structure. Not in place of it.
How Treatment May Be Given
When stem cell or exosome treatment is considered in diabetic nephropathy, patients usually want practical clarity early.
Sometimes treatment is given intravenously.
In some cases, a more targeted route may be chosen, with a thin catheter guided under imaging into the vessels supplying the kidneys. When that route is used, it should be done by an experienced interventional radiologist and only after the anatomy, disease stage, and rationale have been reviewed carefully.
What Patients With Diabetic Nephropathy Usually Hope For
Most are not asking for dramatic transformation.
They are asking for control.
- Control over a process that has already started.
- Control over numbers that keep slipping.
- Control over the fear that kidney disease may become the next major diabetic complication.
And very often, they are asking for time.
- Time before later-stage CKD.
- Time before dialysis enters the vocabulary.
- Time before one chronic disease becomes two.
That is why even modest slowing can matter so much in diabetic nephropathy. To the physician, it may look incremental. To the patient, it often feels much larger than that.
When This Discussion Should Be More Cautious
There are also situations where this whole discussion has to become more restrained.
If kidney scarring is already advanced, if the disease has been active for years without real control, if several other complications are already present, or if the patient expects regenerative therapy to replace diabetic discipline, then the role of these treatments becomes much weaker.
Sometimes the better consultation is the one that sounds more limited.
That is not pessimism.
It is the difference between protecting the patient and performing optimism.
FAQs on Stem Cell Therapy for Diabetic Nephropathy
Can stem cell therapy reverse diabetic nephropathy?
Usually not in the full way patients want it to.
If diabetic kidney damage has already produced clear scarring, the realistic goal is not to make the kidney new again. The more honest goal is to slow the process down, reduce some of the pressure on the tissue, and protect what still works.
Why is diabetic nephropathy discussed so often in regenerative medicine?
Because it is not just one kind of injury.
Diabetic nephropathy is being pushed by several things at once: metabolic stress, vascular injury, inflammation, and fibrosis. That is one reason it keeps appearing in regenerative discussions. The disease itself is biologically active in more than one direction.
Can the kidneys still get worse even if the patient feels fine?
Yes. Very easily.
That is one reason patients are often surprised by the diagnosis. Daily life can still feel fairly normal while the disease is moving through urine changes, filtration loss, and tissue stress in the background.
Is stem cell therapy a substitute for diabetes control?
No.
If blood sugar stays poorly controlled, the kidney is still exposed to the same pressure that helped create the damage in the first place. Regenerative therapy, where it is discussed, can only make sense on top of proper diabetic and kidney care.
Which patients are more realistic candidates for treatment?
Usually the patients who still have enough kidney reserve left that preservation is worth something.
If the disease is active, but not yet completely dominated by advanced scarring, there may still be a stronger reason to discuss treatment seriously. That conversation gets weaker when too much function has already been lost.
Conclusion
Diabetic nephropathy is one of the clearest examples of how chronic disease narrows life slowly.
Not in one dramatic day.
But over time.
That is why it deserves earlier attention than it often receives.
Stem cell therapy for diabetic nephropathy is not a cure, and it should not be described that way. But in selected patients, it may still deserve a serious discussion as part of a broader effort to reduce ongoing injury and protect what remains.
That is the real goal.
Not fantasy.
Not rescue.
Preservation, while preservation is still possible.