CKD vs Kidney Failure: What’s the Difference?
Clinical Insights by Prof. Dr. Serdar Kabataş, MD, PhD (C)
Clinical Perspective on CKD and Kidney Failure
Patients almost never arrive with clean terminology.
They don’t say, “I have stage 3 chronic kidney disease.”
They don’t ask, “Am I approaching end-stage renal failure?”
They say something more immediate.
“My kidneys are weak.”
“Something is wrong with my labs.”
Or quietly: “Will I need dialysis?”
That last question matters.
Because it shows what patients are really trying to understand: not definitions, but direction.
And this is where confusion starts.
Chronic kidney disease and kidney failure are often used as if they mean the same thing. They do not. One describes a process. The other describes what happens when that process has gone far enough.
If you miss that distinction, everything else becomes harder to interpret — prognosis, treatment, even hope.
Table of Contents
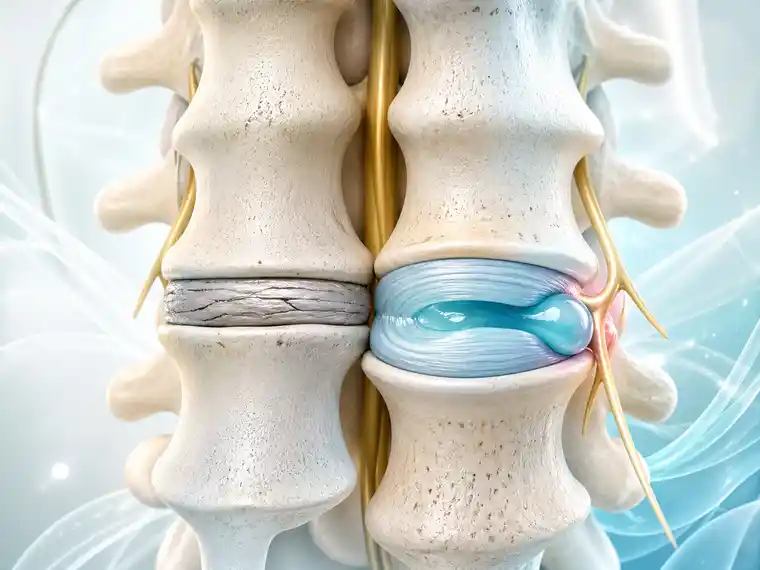
What Chronic Kidney Disease (CKD) Actually Means
Chronic kidney disease is not a single diagnosis in the way many patients imagine it.
It is a framework.
A way of describing that the kidneys are either structurally damaged or functionally reduced over time.
That “over time” is important.
CKD is not an event. It doesn’t really begin in a way people can point to.
There’s no clear first day. No moment where someone says, this is when it started. It’s usually something that has been building in the background for quite a while.
Most patients feel completely normal at first. Maybe a lab value is slightly off, but it doesn’t interrupt daily life. Nothing forces attention. That’s one of the reasons chronic kidney disease is so often picked up late — not because it’s rare, but because it doesn’t announce itself.
Even later, the situation can still feel surprisingly stable.
The kidneys may already be under pressure, filtering less efficiently, struggling a bit more with fluid balance or waste products. But the body is very good at compensating. It adjusts quietly, sometimes for longer than patients expect.
That’s also why we use stages.
Not because something dramatic happens between them, but because they give us a rough sense of how much functional reserve is still there — and how much margin is starting to disappear.
And in many patients, that reserve lasts for years.
What Kidney Failure Means
Kidney failure is different in one important way.
It is no longer about reduced function.
It is about insufficient function.
This is usually what we refer to as stage 5 CKD — the point where the kidneys can no longer maintain the internal environment the body depends on.
Waste products accumulate.
Fluid balance becomes unstable.
Electrolytes shift in ways that can affect the heart, the brain, and overall stability.
At that stage, the body needs support.
Not optional support, but necessary support — through dialysis or kidney transplantation.
This is why kidney failure is not just “advanced CKD.”
It is the point where compensation is no longer enough.
CKD vs Kidney Failure: The Core Difference
The distinction becomes clearer when you step back.
Chronic kidney disease describes a continuum.
Kidney failure describes a threshold.
CKD means the kidneys are not working as they should.
Kidney failure means they can no longer do what the body requires.
Or more simply:
CKD is the process.
Kidney failure is what happens when that process reaches its limit.
That difference may sound semantic, but for patients it is anything but.
Because it defines whether the situation is still adjustable – or already dependent on replacement therapy.
Why Patients Often Confuse the Two
Patients do not experience kidney disease as stages or categories. They experience it as uncertainty.
- A lab value changes.
- A doctor mentions “reduced function.”
- Medication is adjusted.
- At some point, the word “kidney” enters the conversation — and with it, the fear of dialysis.
- From the outside, everything begins to blur.
- But medically, there is a large distance between early CKD and kidney failure.
And that distance is where most decisions actually matter.
How CKD Progresses Toward Kidney Failure

Progression is not automatic in chronic kidney disease.
This is one of the most important points – and one of the most misunderstood.
Not every patient with CKD will develop kidney failure.
Some remain stable for many years. Others decline slowly. A smaller group progresses more quickly.
What determines that difference is not one factor, but several acting together:
- persistent high blood sugar
- poorly controlled blood pressure
- vascular damage
- chronic inflammation
- repeated metabolic stress
Over time, these pressures affect the small filtering structures of the kidney. The tissue adapts, compensates, and eventually begins to scar.
That scarring – fibrosis – reduces functional capacity further.
And once that process is established, it tends to continue unless the underlying drivers are brought under control.
Can CKD Be Slowed Before Kidney Failure?
This is usually the moment where the conversation becomes practical.
Because patients are not asking for definitions anymore.
They are asking for influence.
In many cases, progression can be slowed.
Sometimes significantly.
But that depends less on the label and more on the situation:
- How early was the disease detected?
- Is the underlying cause still active?
- Are blood sugar and blood pressure controlled?
- Is follow-up consistent?
The goal is not to “reset” the kidneys.
That is not realistic once structural changes have occurred.
The goal is to preserve function — to keep the decline as slow as possible for as long as possible.
For many patients, that changes everything.
Where Regenerative Therapy Enters the Discussion
In recent years, another question has started to appear more frequently.
Not whether kidney disease can be reversed.
But whether the environment in which the damage continues can be influenced.
This is where chronic kidney disease stem cell therapy, including stem cells and exosomes, enters the discussion.
Not as a replacement for standard nephrology care.
And not as a cure.
But as a possible way to affect inflammation, signaling pathways, and cellular behavior within the kidney.
The idea is not to rebuild an organ.
It is to reduce ongoing injury.
That distinction matters.
Because it keeps expectations realistic — and the discussion medically grounded.
When CKD Becomes Kidney Failure
There are situations where, despite all efforts, kidney function continues to decline.
At a certain point, the remaining function is no longer sufficient.
This is where the conversation changes.
It becomes less about slowing progression and more about maintaining stability.
Dialysis is introduced.
Transplantation becomes a consideration.
And the question is no longer “How do we prevent this?”
It becomes: “How do we support the body now?”
That is the reality of kidney failure.
Conclusion
Chronic kidney disease and kidney failure are part of the same continuum, but they are not the same condition.
One describes a process that develops over time.
The other describes the point where that process has reached its limit.
For patients, that distinction matters because it defines what is still possible.
In earlier stages, there is often room to slow the disease.
In later stages, the focus shifts to support and replacement.
Understanding where you are in that spectrum is not just informative.
It is the basis for every meaningful decision that follows.
FAQs About CKD vs Kidney Failure
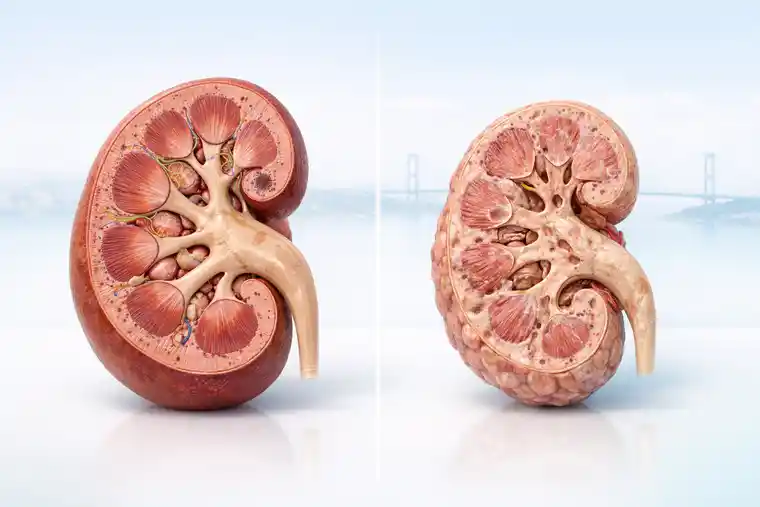
Is chronic kidney disease already kidney failure?
No. And this is probably the most common misunderstanding I see.
When we say “chronic kidney disease,” we are often talking about a long phase where the kidneys are still working — just not at full capacity. That can go on for years. Kidney failure is a different situation. That is the point where the remaining function is simply not enough anymore.
So the two are related, but not interchangeable.
If someone has CKD, is dialysis basically inevitable?
No, not at all.
There are patients I have followed for a long time whose kidney function is reduced, but stable. Nothing dramatic happens. Then there are others where the numbers slowly move in the wrong direction.
The important part is not the label “CKD.”
It is the behavior of the disease over time.
When do doctors actually start talking about kidney failure?
Usually not after one lab result.
It becomes a real topic when several things come together — declining filtration, symptoms, and the sense that the body is no longer compensating the way it used to. That is often around what we call stage 5, but even then, timing is individual.
There isn’t a single number where everything suddenly changes.
Can you still influence the course once kidney disease has started?
Yes, in many cases.
But not in a dramatic, overnight way. It is more about direction than reversal. When blood pressure is controlled, when diabetes is managed properly, when follow-up is consistent — the slope can change.
Patients sometimes underestimate how much that matters over years.
Why do so many people only find out late?
Because nothing really forces the issue early on.
The kidneys compensate quietly. People feel fine, or at least fine enough not to think about it. And then one day there is a lab result that no longer fits.
When you look back, the process has usually been there for quite a while.
What about stem cells or exosomes — are these already part of standard treatment?
No.
They come up more often now, especially in discussions about slowing progression. But they are not a replacement for established care, and they are not routine treatment.
If they are considered at all, it is usually in a very specific context — and always on top of standard management, not instead of it.
Get your free consultation
- Need guidance and reassurance?
- Talk to a real person from MedClinics!
- Let's find the perfect doctor together.